This article first appeared in The Havok Journal on 14 August 2014.
_____
Osteoporosis is a debilitating disease characterized by an overall loss of bone density that is incredibly common but also preventable.
The scary part is that it’s uncommon for the disease to be diagnosed before clinical symptoms appear. Once those clinical symptoms appear, you are already at an advanced stage of the disease and there is nothing that can be done to repair the damage. At this point, the best treatments available are, at best, only going to keep the problem from getting worse. Osteoporosis is most common in post-menopausal women.
Therefore, if you are a post-menopausal woman, or are a woman who will become post-menopausal, it is imperative that you take notice. If you are in some way close to a woman who is, or will become post-menopausal, it is in your best interest to also educate yourself on the causes, effects, and ways to prevent osteoporosis. In other words, this is relevant to just about everyone so keep reading.
The first step necessary in preventing a disease is to understand the disease. What is osteoporosis? Why does bone density decrease as we age? Why are women more affected than men? Why does it mainly affect women after they’ve gone through menopause? The answers to most of these questions lie on a cellular level, and we’ll have to explore a little bit of this before we move on. If you’ve never taken a day of cell biology in your life, do not despair. We’re going to try and make this as simple as possible to understand. I find it very beneficial to have pictures to reference while reading, so I’ve drawn a few to aid in understanding some of the cell biology; please refer to them as needed.
Osteoporosis is a disease that is characterized by an overall loss of bone density that makes the bones brittle and more likely to break. In a normal person, there is a balance (known as homeostasis) in the bone remodeling process between breaking down bone (degradation) and building bone. Osteoporosis occurs when bone degradation overwhelms your body’s ability to build new bone. If left unchecked, the bone loss becomes severe and results in osteoporosis.
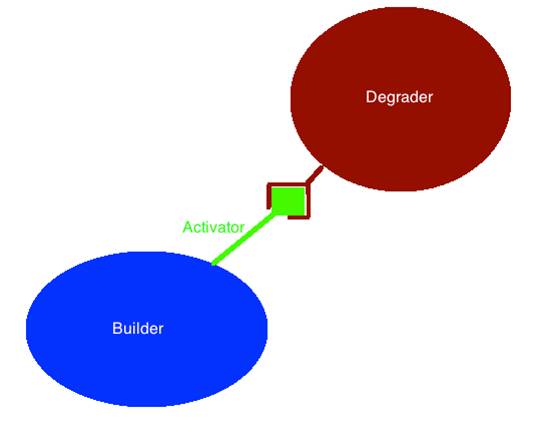
There are essentially two major types of cells that are responsible for bone remodeling. These cells are called osteoblasts, which are bone builders, and osteoclasts, which are responsible for breaking down bone. Now, I’m sure some of you glazed over as soon as I started naming cells, so for simplicity and to limit the medical jargon, I’ll from now on refer to these as builders and degraders.
There is a strange interplay between the builders and the degraders in the body. When the builders are working, they exhibit a chemical that activates the degraders. The reason why the degraders are activated along with the builders is partly because you can’t have construction without a little bit of destruction. It is the degraders’ job to break up some of the old bone in order to make way for the new bone.
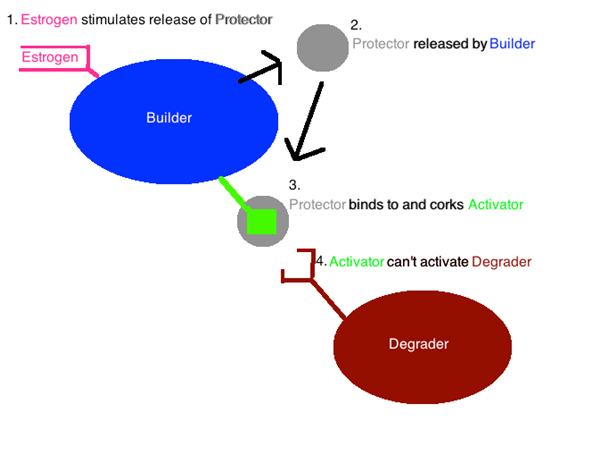
The trick to the whole process is the ability to activate the builders without activating the degraders when the time for demolition has passed and it’s time to build new bone. This trick is performed by a molecule called osteoprotegrin (from here on out referred to as the protector). This chemical is also released by the builders, but is done in response to estrogen outside of the cell. This molecule acts as a cap that covers up the activator and keeps it from activating the degraders. It fits on the end of the activator like a cork, and keeps it from activating the degraders.
I mentioned earlier that the protector is released in response to estrogen. Herein lies the link between osteoporosis and menopause. When a woman hits menopause, there is a sharp decline in the amount of estrogen her body produces. Without the proper levels of estrogen, there are not enough protectors to go around, and more degraders are subsequently activated and left free to go nuts.
(Continued on Next Page)
Buy Me A Coffee
The Havok Journal seeks to serve as a voice of the Veteran and First Responder communities through a focus on current affairs and articles of interest to the public in general, and the veteran community in particular. We strive to offer timely, current, and informative content, with the occasional piece focused on entertainment. We are continually expanding and striving to improve the readers’ experience.
© 2026 The Havok Journal
The Havok Journal welcomes re-posting of our original content as long as it is done in compliance with our Terms of Use.