She looked at me like I was already gone.
I think she was a radiology technician student—young, awkward, and working alongside an older, grizzled tech whose eyes were dulled by routine.
“You… you should get your… results in about three days, sir,” she said. Her words trembled.
Unlike her preceptor—an experienced professional who supervises and mentors clinical trainees—she couldn’t hide her empathy.
I had Covid in January 2020—before we knew what Covid was. Like so many, I burned with fever, and my lungs filled with mucus for days. I coughed so much my abdominal muscles cramped from overuse. I pounded my chest to break up secretions… I didn’t want pneumonia settling in. Once, I was close to asking Jennifer—my wife—to take me to the hospital. It seemed I could only get the upper portion of my lungs to inflate; the rest were inflamed and fluid-filled.
But I eventually recovered and pressed on with life. Except on my runs, it seemed I never quite bounced back. I chalked it up to getting old—and to “long Covid.” But when August 2020 came and I still hadn’t improved, I did something I’d never done before. I called my PCM and made an appointment.
Initial imaging escalated quickly—from chest X-ray to CT to biopsy—all pointing to something more serious. It was during the CT that I met that radiology student whose look made my ears perk up.
That CT revealed multiple concerns—thyroid calcification, lung nodules, and possible liver lesions. I was immediately referred to ENT. I was going to need a liver CT and a repeat chest CT in three months to see if the lung nodules were stable.
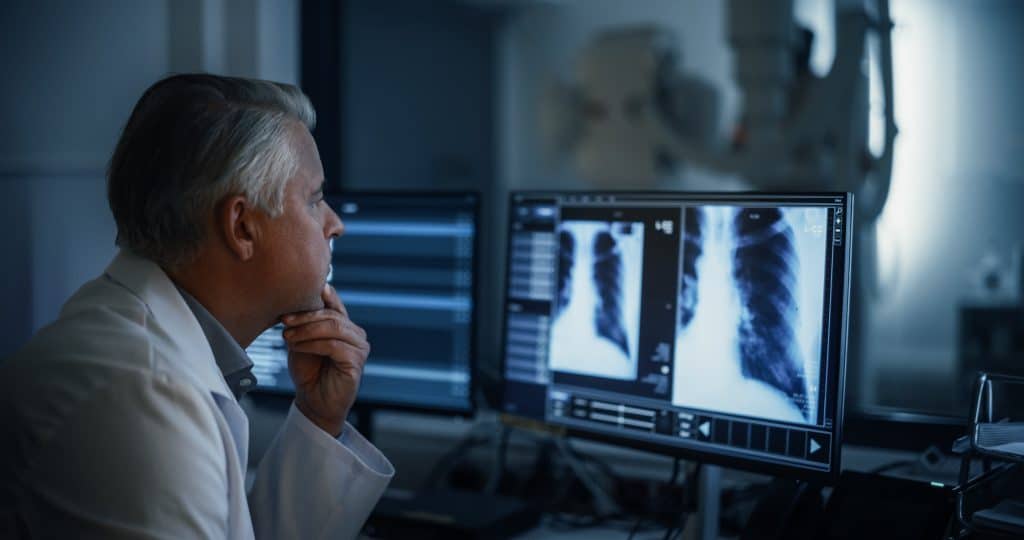
Thankfully, the follow-up liver CT showed multiple cysts—benign, most likely congenital. A blood test later confirmed no hepatitis or parasitic infections.
A week or two later, I had an ultrasound of my neck, which showed I most likely had thyroid cancer. But I couldn’t be scheduled for surgery without a biopsy to confirm this—and it took three weeks to get the biopsy because Covid had slashed appointments for procedures.
It was a long three weeks.
When the ENT surgeon called to schedule an appointment the next day to “discuss my results,” I told Jennifer if the results were good, the surgeon would’ve told me over the phone—and that I’d be scheduling surgery ASAP.
The surgeon gave me the news and said she recommended a total thyroidectomy as soon as possible. There was also a risk of having all four parathyroid nodes removed in the process—those regulate calcium in the body—meaning I might have to take calcium supplements along with Synthroid (a thyroid hormone replacement) for the rest of my life.
I think the surgeon expected more reaction from me. But it was November 2020. By that point, we’d known something was up for more than two months and that I had thyroid cancer for almost a month.
“You’re the first person I’ve talked to that can do something about it,” I told her.
Up until that point, we’d just ruled out liver cancer. A repeat chest CT was scheduled the next month to see if the lung nodules had changed.
Thoughts of my dad’s death from lung cancer hung ominously—he’d been diagnosed in this very same hospital eight years earlier.
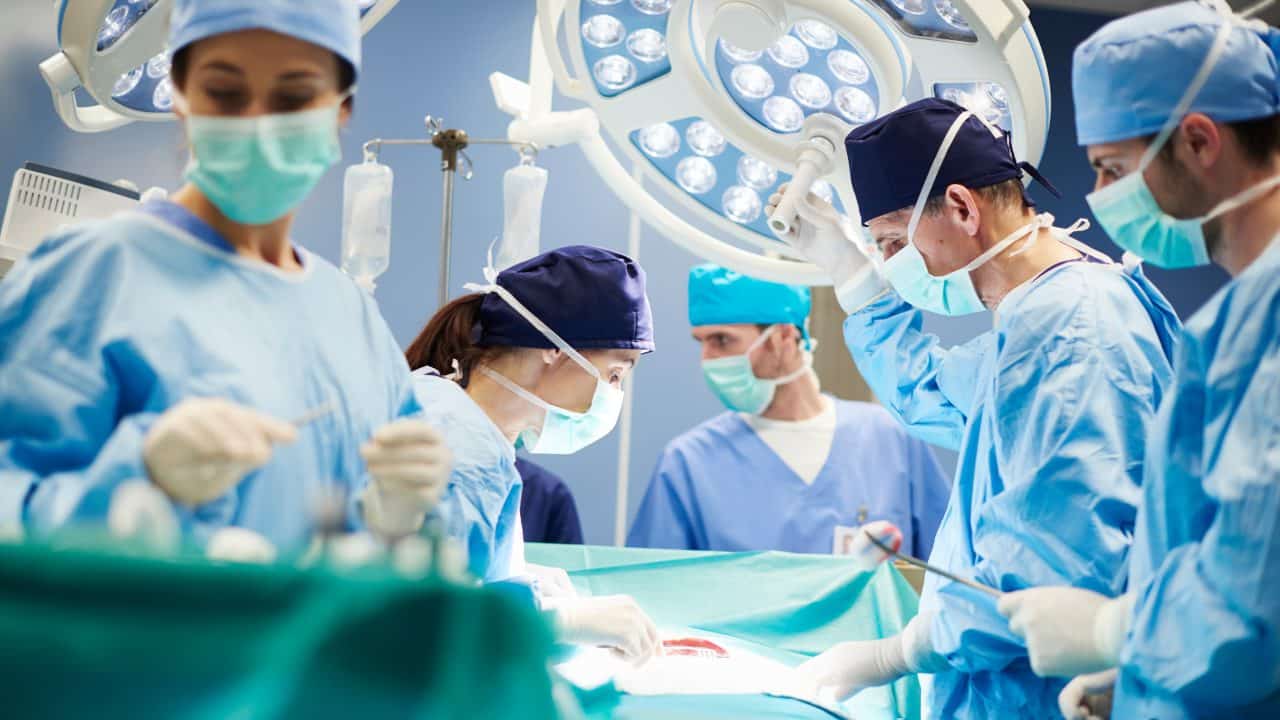
I’d worked in Operating Rooms (OR) from 1995–2013 and was the Clinical OIC of the OR at Womack Army Medical Center from 2010–2012. It was the very OR where I’d have my thyroidectomy. I was past the point of chomping at the bit to get this done.
My surgery was scheduled for mid-November. I had a neck CT with contrast to check if the cancer had spread to any neck lymph nodes. I breathed a sigh of relief when the radiologist’s report indicated no findings. Adding to the stress was the fact that my son had Covid during this time, and if I’d tested positive, my surgery would’ve been postponed.

I received a phone call the weekend before my surgery. Although the radiologist cleared my neck CT, the ENT surgeon saw something she thought might be cancer in one of the neck lymph nodes. Again, they needed a biopsy to confirm it.
As I drove to Womack, the experience was surreal. I’d never been a patient there—only staff. When I arrived at the ENT clinic, my surgeon and a partner ENT surgeon were there—along with lab staff. The surgeon performed a fine needle aspiration on one of my neck lymph nodes, and the lab examined it right there in the room.
The look on his face confirmed it: the cancer had spread.
The surgeons did their best to warn me of all the possible outcomes—ranging from death and nerve damage to needing calcium and Synthroid for the rest of my life.
I didn’t care—I trusted them. I would sign whatever consent form they put in front of me.
It was no longer only a total thyroidectomy. It would now include central neck levels VI and VII plus right level I, II and IV lymph node dissections—what ended up being 40 lymph nodes.
I remarked that it felt like I was dodging a bullet in slow motion. I’ll never forget one of the staff’s quips: “Just keep dodgin’, sir.”
I’d wondered if I had liver cancer a month earlier. I still wondered if I had lung cancer. With Covid still rampant, I prayed just to stay clear long enough for surgery.
I went through our finances with Jennifer—everything she’d need to carry forward if I wasn’t in the picture. She took notes, asked questions, nodded quietly. There was a steadiness in her I didn’t fully recognize at the time. The only crack came once, when we passed Sandhills State Veterans Cemetery. She asked, almost casually, “Would you want to be buried next to your dad?”
I told her to do whatever was cheapest. My biggest concern was not leaving her with a financial burden. That was the cold reality.

I hadn’t slept well in months. Nightmares, fears, death. Covid. The unknowns piled up—test after test, scan after scan. A long road ahead. I would need radioactive iodine (RAI) after surgery to, hopefully, kill any residual cancer—and more imaging to see if it had spread to my lungs.
I found out that two civilian nurses who had worked for me during my active duty time—Terry Murray and Kay Chavis—were going to be working my case. I knew them well. Not only were they two of the most capable OR nurses I’d ever known, they were also two of the wisest people I’d known. I took such solace knowing they were going to take care of me. It was the first time I felt a measure of peace.
I was contacted by a tumor coordinator who wanted me to be part of a government study. I was an otherwise healthy male in my late 40s with fairly advanced thyroid cancer who’d served in Iraq. I hated filling out the forms because it made it more real. I thought of all the burn pit smoke I’d been exposed to in 2004. I felt obligated to be part of this study. It might help other veterans. But I didn’t want to be contacted in the future—I didn’t want to know what they found.
I’d retired from the Army in July 2019 and was scared and angry at the prospect of making it through 20 years of military service only to die shortly after. I wasn’t alone. I was a statistic. Other veterans were facing the same—or worse.
I’d told my surgeon: “I’m not worried about the surgery. I’m worried about what comes after it.” Because I’d need radioactive iodine treatment, and follow-up for years to ensure there was no recurrence. We also didn’t know what the next chest CT would show.
When Jennifer drove me to Womack for my surgery—I couldn’t have been more thankful for that building being there. I was utterly dependent on it for saving my life. I’d never felt so vulnerable.
As I dropped off my consent forms to the tumor coordinator, I signed final paperwork and couldn’t help but think of the beginning scene in Terminator Salvation, when the protagonist is about to be put to death and signs forms donating his body to research.
Jennifer and I checked in. Due to Covid protocol, she couldn’t go with me to pre-op holding. I held her. I kissed her. I told her I loved her.
As I was escorted away, she cried quietly. There was a moment I could feel what I can only describe as a “behind-the-scenes” power—as if there was a peeling of the veil of reality. It felt ancient and eternal, an aching, overwhelming love. I didn’t want to leave Jennifer.

I belonged with her.
It was strange to be a patient in an OR I’d once worked in and ran myself. Some of the same civilians were still there. It was familiar. I knew how it worked—its complexities, the drama, and the hard work that went into making surgery happen.
As I was wheeled into the OR, the nurse anesthetist said, “You may not remember me, but you were my Assignment Officer.” I tensed, unsure where it was going, as Assignment Officers are often reviled for sending soldiers to places they don’t want to go. He continued, “I just wanted to thank you. You helped with my report date from Korea and made sure my replacement arrived on time. That meant a lot.”
I breathed a quiet sigh of relief.
They strapped me down on the OR table. For the first time, I was on the receiving end—and, like so much of this experience, it was like being in a dream. Again, seeing Terry and Kay was a godsend. I trusted my surgeons, I trusted the OR team. I was in good hands.
As I lay looking up at the ceiling, I thought of the years I’d spent in that very OR. The people past and present. They had no idea how much I loved and respected them. It was the most meaningful military assignment I’d ever had—and the last time I’d worked in an OR.
I’d had three PCS moves after leaving Womack in 2012. Yet somehow, here I was—back in the same OR, placing my life in the hands of the very system I once helped run.
As they placed the mask on me to preoxygenate, I thought: What were the odds that I’d end up on this OR table? Somehow, I knew it was meant to be. There was no other OR I wanted to be in. Even if I died, I was glad it was here.
“You might feel some burning in your IV,” said the anesthetist. He was about to push a bolus of propofol. It renders patients unconscious—so that they can be intubated.
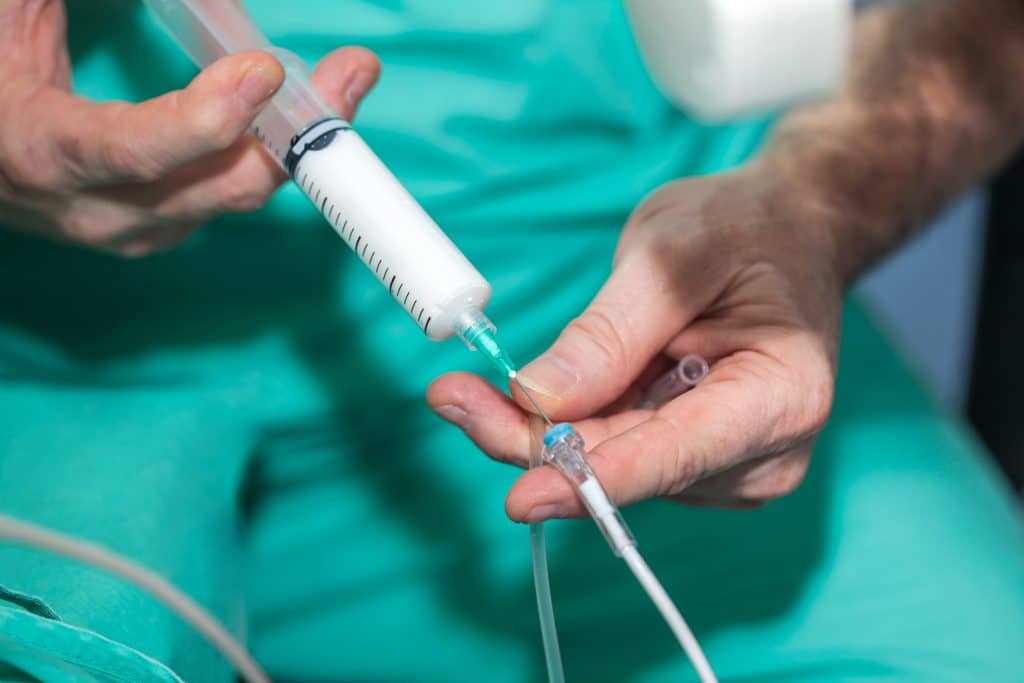
“I want you to count backwards from 10 to 1.”
“10,” I said.
I didn’t want to leave this life.
“9.”
I wanted to see my children grow into adults.
“8.”
I wanted to be with my wife.
“7.”
I didn’t want to lose her.
I never got to six.
There was still so much I needed to be here for.
I woke up in recovery. I would spend the next two days in the hospital—mainly to monitor my calcium levels. If I had no parathyroid left, they could drop dangerously low, leading to life-threatening neurological or cardiovascular issues.
My ENT surgeon checked on me. She told me she’d spoken with Jennifer and that the surgery went very well. The surgeon remarked that Jen had asked many astute questions.
She then leaned forward, her tone severe—“Your wife really loves you.”
The way she said it pierced the moment. I could hear it in her voice. Her tone told me she’d seen Jennifer’s love for the rare and beautiful thing it is.
I thought of the preceding three months. The scans. The labs. The uncertainty. And now the surgery. I hadn’t seen it—not really. I’d been too wrapped in the storm.
It wasn’t until the surgeon said, “Your wife really loves you,” that I stopped paying attention to the fear. And saw that Jennifer had quietly borne those same burdens with strength and grace every step of the way.
There would be more tests. More treatment. More imaging. More diagnoses.
I thought I was the one dodging bullets. But Jennifer was there too—still, silent, unflinching.
That’s my lament. I was too scared to notice… until then.
The bravest thing I never saw.
________________________________
Mike Warnock is the editor-in-chief of The Havok Journal and a retired U.S. Army Major and Air Force veteran with 20 years of active service across both branches. During his career, he led surgical teams as an Operating Room Officer-in-Charge at the hospital, medical center, and combat-support levels, later serving in senior clinical, administrative, and inspector general roles before retiring in 2019. Over his 23-year civilian and military nursing career, he deployed to Guam and twice to Iraq, leading surgical and clinical teams in both peacetime and combat environments. He holds a B.S. in Nursing from the University of North Carolina at Charlotte and an M.A. in Military History from Norwich University.
As the Voice of the Veteran Community, The Havok Journal seeks to publish a variety of perspectives on a number of sensitive subjects. Unless specifically noted otherwise, nothing we publish is an official point of view of The Havok Journal or any part of the U.S. government.
Buy Me A Coffee
The Havok Journal seeks to serve as a voice of the Veteran and First Responder communities through a focus on current affairs and articles of interest to the public in general, and the veteran community in particular. We strive to offer timely, current, and informative content, with the occasional piece focused on entertainment. We are continually expanding and striving to improve the readers’ experience.
© 2026 The Havok Journal
The Havok Journal welcomes re-posting of our original content as long as it is done in compliance with our Terms of Use.