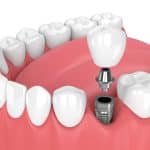
The procedure for single tooth implants is a meticulous process that demands precision and expertise. It begins with an in-depth consultation and evaluation to assess the patient’s oral health. A personalized treatment plan is crafted, considering factors such as bone quality and oral hygiene. Each stage, from tooth extraction to implant placement and crown attachment, is vital. Comprehending these steps is indispensable to appreciate the implant’s complexity and guarantee its successful integration.
Initial Consultation and Evaluation
During the initial consultation and evaluation for a single tooth implant, the dental professional conducts a thorough assessment of the patient’s oral health status to determine candidacy for the procedure. This process involves a comprehensive examination, which includes a detailed review of medical and dental history, clinical evaluation, and diagnostic imaging techniques such as X-rays or CT scans. The oral health assessment focuses on identifying any underlying conditions that could impact the success of the implant, such as periodontal disease, bone density, and overall oral hygiene. The practitioner evaluates the integrity of the surrounding teeth and the quality of the jawbone to ascertain it can support the implant. This meticulous evaluation is vital for formulating an effective treatment plan tailored to the patient’s specific needs.
Treatment Planning and Preparation
In the treatment planning and preparation phase for single tooth implants, a thorough patient assessment process is vital to determine individual needs and anatomical considerations. Advanced imaging and diagnostics, such as cone beam computed tomography, are employed to obtain detailed visualizations of the oral structures, facilitating precise implant placement. Patients considering affordable single tooth implants in Long Beach can benefit from these personalized evaluations, which help ensure ideal functional and aesthetic outcomes tailored to their specific clinical situation.
Patient Assessment Process
How does one assure the ideal outcome for a single tooth implant? The process begins with a comprehensive patient assessment. Evaluating the patient medical history is paramount, as it identifies systemic conditions like diabetes or osteoporosis that may affect healing and osseointegration. A meticulous examination of patient oral health is essential, appraising periodontal status, gum health, and the presence of any infections or oral diseases. This includes the evaluation of the quality and quantity of the alveolar bone in the intended implant site. Additionally, evaluating the patient’s oral hygiene practices guarantees they can maintain the implant postoperatively. By integrating these assessments, a tailored treatment plan can be devised, maximizing the probability of implant success and long-term functionality.
Imaging and Diagnostics
To guarantee accurate treatment planning and preparation for a single tooth implant, imaging and diagnostics play a pivotal role. Radiographic analysis is essential to assess bone quality and quantity, ensuring the implant’s stability and longevity. Digital impressions provide a precise 3D model of the oral cavity, allowing for meticulous planning of the implant’s position and angle. The following components are integral to the imaging and diagnostic process:
- Cone Beam Computed Tomography (CBCT): Offers detailed 3D images of the jawbone structure, critical for evaluating bone density and detecting anatomical variations.
- Panoramic X-rays: Provide an extensive view of the mouth, aiding in the identification of any underlying dental issues.
- Intraoral Scanners: Capture highly accurate digital impressions without the discomfort of traditional molds.
- Diagnostic Models: Facilitate visualization and analysis of the implant site within the context of the entire dentition.
Customized Treatment Plan
After obtaining thorough imaging and diagnostic data, a customized treatment plan becomes imperative for the successful placement of a single tooth implant. Implant customization is predicated on precise patient-specific considerations, which include bone density, anatomical landmarks, and occlusal forces. The treatment plan must evaluate the optimal implant size, shape, and positioning to guarantee functional integration and aesthetic alignment. Clinicians assess the adjacent teeth and gingival contour to tailor the implant’s restorative design. Advanced software aids in simulating the implant placement, enhancing predictability and reducing procedural risks. Collaboration with dental technicians allows for the creation of a prosthesis that seamlessly integrates with the patient’s oral environment, consequently ensuring longevity and comfort. The customized treatment plan is pivotal in achieving desired outcomes.
Tooth Extraction and Site Preparation
When considering the initial phase of single tooth implant procedures, tooth extraction and site preparation are critical steps that require meticulous attention to detail. The extraction technique employed must minimize trauma to the surrounding bone and soft tissue, facilitating ideal healing. Following extraction, site preparation may involve bone grafting to enhance bone density and provide a stable foundation for the implant. The process involves several key steps:
- Assessment: Evaluate the site for existing bone volume and quality.
- Extraction: Employ atraumatic techniques to preserve alveolar bone structure.
- Bone Grafting: Utilize autogenous bone or synthetic materials to augment deficient areas.
- Site Healing: Allow sufficient time for graft integration and soft tissue recovery before implant placement.
These steps guarantee a suitable environment for the upcoming implant procedure.
Implant Placement Surgery
Implant placement surgery begins with meticulous surgical site preparation, ensuring ideal conditions for implant stability. The implant insertion process involves precise drilling techniques to place the titanium post into the jawbone, aligning it accurately with the surrounding structures. Post-surgery, a defined healing and recovery period is essential, allowing osseointegration to occur and ensuring the long-term success of the implant.
Surgical Site Preparation
The preparation of the surgical site is a critical step in implant placement surgery, demanding meticulous attention to detail to safeguard ideal results. This involves guaranteeing the site is structurally capable to support the implant. Essential steps include:
- Assessment of Bone Quality: Evaluating bone density and volume to determine if bone grafting is necessary.
- Bone Grafting: When insufficient bone is present, grafting material is applied to enhance the site.
- Site Contouring: Precise shaping of the bone surface to create a stable and contoured foundation.
- Sterile Field Establishment: Ascertaining a contamination-free environment to prevent infection.
Each step is meticulously executed to guarantee the implant’s stability and longevity, providing a robust base for the subsequent implant insertion process.
Implant Insertion Process
After the surgical site has been meticulously prepared, the implant insertion process begins with the careful placement of the dental implant into the jawbone. The dental professional uses a specialized drill to create a precise osteotomy that matches the dimensions of the implant. This guarantees optimal implant stability, a critical factor in successful osseointegration. The implant is then gently screwed into the prepared site. Torque control is paramount to avoid excessive force that could compromise the surrounding bone. Once positioned, the implant must achieve primary stability, meaning it is securely held in place by the surrounding bone. This stability is essential for the process of osseointegration, where the bone gradually fuses to the implant surface, ensuring long-term success of the dental implant.
Healing and Recovery Time
Following the placement of a dental implant, a pivotal period of healing and recovery commences, during which the body begins the complex process of osseointegration. This process typically spans several months, influenced by individual patient factors. The recovery timeline can be optimized through careful adherence to post-operative guidelines. Key considerations include:
- Osseointegration Duration: The implant integrates with the bone over 3 to 6 months, depending on bone quality and patient health.
- Dietary Considerations: Soft foods are recommended initially to minimize stress on the implant site.
- Inflammation Management: Patients may experience mild swelling; anti-inflammatory medications are often advised.
- Follow-up Appointments: Regular dental visits are essential to monitor healing progress and confirm proper implant stability.
Adhering to these factors aids in successful recovery and implant longevity.
Healing and Osseointegration Period
How long does it take for a single tooth implant to fully integrate with the jawbone? The integration period, termed osseointegration, typically spans 3 to 6 months. This duration allows for tissue integration and bone regeneration, critical processes where the surrounding bone gradually fuses with the implant. During this phase, osteoblast cells play a pivotal role in forming new bone around the implant, guaranteeing stability and support. The implant surface encourages tissue integration, promoting the attachment of gingival tissues. This meticulous process certifies the implant becomes a functional part of the oral structure. Factors such as the patient’s bone quality, oral hygiene, and systemic health can influence the osseointegration period, dictating the success of the implant’s long-term performance.
Abutment Placement
With osseointegration complete, the next phase involves the precise placement of the abutment, the intermediary component that connects the dental implant to the prosthetic crown. This pivotal step requires meticulous consideration to guarantee optimal function and aesthetics. Key factors include:
- Abutment Selection: The choice of abutment—standard or custom—depends on the specific anatomical and clinical requirements of the patient.
- Abutment Customization: Custom abutments are tailored to a precise fit, enhancing the alignment and contour of the final restoration.
- Abutment Height and Angulation: Proper adjustment of height and angulation is essential for achieving the desired occlusion and comfort.
- Tissue Compatibility: The selected material should ensure biocompatibility, minimizing the risk of adverse tissue reactions.
These factors collectively guarantee the abutment’s successful integration and functionality.
Designing and Creating the Dental Crown
Once the abutment is securely in place, the focus shifts to designing and creating the dental crown, the final component that restores both function and aesthetics to the implant site. Crown design begins with a digital or physical impression of the patient’s dentition, guaranteeing precise fit and occlusion. The design process incorporates aesthetic considerations, including shade matching and translucency, to harmonize with adjacent teeth. Advanced CAD/CAM technology often aids in crafting a crown from materials such as porcelain or zirconia, known for their strength and resemblance to natural enamel. Technicians meticulously shape the crown, addressing functional requirements like bite force distribution. This technical precision confirms the dental crown complements the patient’s oral environment while maintaining natural aesthetics and durability.
Crown Attachment and Final Adjustments
The final phase in the dental implant process involves attaching the meticulously crafted crown to the abutment, ensuring a seamless and stable integration. This stage requires precision to address crown customization and esthetic considerations effectively. The dental professional assesses the crown’s fit and alignment, making necessary adjustments for ideal function and appearance.
Key steps include:
- Verification of Fit: Ensuring that the crown aligns perfectly with adjacent teeth and the opposing bite.
- Esthetic Evaluation: Checking the color, shape, and size of the crown to match natural teeth, maintaining harmony in the dental arch.
- Cementation Process: Using dental cement to secure the crown, prioritizing durability and strength.
- Final Adjustments: Minor modifications to the crown’s occlusion and contour for patient comfort and functionality.
Post-Operative Care and Maintenance
After the crown is securely attached, diligent post-operative care and maintenance are crucial to guarantee the longevity and health of a single tooth implant. Patients are advised to follow specific diet recommendations, initially avoiding hard and sticky foods that may compromise the implant’s stability. As the healing progresses, a gradual reintroduction of these food types can be considered under professional guidance. Regular hygiene appointments are indispensable, ensuring thorough professional cleaning and examination of the implant site. These visits facilitate early detection of potential issues such as peri-implantitis. Patients must adhere to a meticulous oral hygiene routine, including brushing with a soft-bristle toothbrush and using interdental brushes or floss. Such measures are essential in maintaining the implant’s structural integrity and overall oral health.
Frequently Asked Questions
What Are the Costs Associated With Single Tooth Implants?
The costs associated with single tooth implants include dental material costs, which vary based on the implant’s material, and implant maintenance fees. These fees encompass professional cleaning, potential adjustments, and periodic evaluations to safeguard the implant’s longevity and functionality.
Are Single Tooth Implants Covered by Dental Insurance?
Single tooth implants may not be fully covered by dental insurance due to coverage limitations and pre-existing condition requirements. Policies often vary, necessitating thorough review to understand specific exclusions and the extent of financial support provided.
How Long Do Single Tooth Implants Typically Last?
Single tooth implants typically last 15 to 25 years, influenced by longevity factors such as bone density, oral hygiene, and implant maintenance requirements. Regular dental check-ups and proper care extend the implant’s lifespan, ensuring ideal functionality and durability.
Can Single Tooth Implants Be Done for Teenagers?
Single tooth implants for teenagers are generally approached with caution due to adolescent development. Oral health implications include potential interference with jaw growth. Detailed assessment by dental professionals is essential to determine suitability and timing for such procedures.
Are There Any Dietary Restrictions After Getting a Single Tooth Implant?
Yes, dietary restrictions often include soft food recommendations to support the implant healing process. Patients are advised to avoid hard, crunchy, or sticky foods to prevent stress on the implant site and guarantee proper osseointegration.
Buy Me A Coffee
The Havok Journal seeks to serve as a voice of the Veteran and First Responder communities through a focus on current affairs and articles of interest to the public in general, and the veteran community in particular. We strive to offer timely, current, and informative content, with the occasional piece focused on entertainment. We are continually expanding and striving to improve the readers’ experience.
© 2026 The Havok Journal
The Havok Journal welcomes re-posting of our original content as long as it is done in compliance with our Terms of Use.