Tranexamic Acid (TXA): Does It Really Make a Difference?
by Andrew Fisher
Bleeding continues to be the leading cause of preventable death in combat. Even with all the medical advances and the ubiquitous use of extremity tourniquets has not been able to save everyone. There are wounds, where a tourniquet cannot be applied and we cannot apply pressure against a bone to compress the artery that is bleeding. These wounds are in the thorax and called non-compressible torso hemorrhage (NCTH). We can now give blood at the point of injury, but is there something else we are doing that can help?
Tranexamic Acid or TXA is a drug administered for a variety of reasons. In Japan, women can by it over the counter for heavy menstrual bleeding. It is used for prophylaxis before some knee surgeries to prevent bleeding. In the military, it is used as an antifibrinolytic, which means it stops the breakdown of clots that have formed at the site of wounds. It has been used for several years in the Role III hospitals in Afghanistan and was added to the Tactical Combat Casualty Care (TCCC) guidelines by the Committee on TCCC in 2011. Like many things in the DoD logistics system, it was not widely distributed at first. It was used by special operations units and slowly made its way to the conventional units for use.

A clot in the body is made up of platelets, several types of chemicals called clotting factors, and fibrin. Fibrin is an insoluble protein that is made from fibrinogen. Fibrinogen, is modified into fibrin by another chemical thrombin.
TXA is a synthetic derivative of the amino acid lysine, it inhibits the breakdown of fibrin by blocking the amino acid lysine site on plasminogen. Plasminogen is a precursor chemical in the body, that is cleaved to plasmin by tissue plasminogen activator (tPA). If tPA sounds familiar, it is the basis for some “clot busting” drugs used in some types of strokes. The plasmin then breaks down fibrin. Therefore, by blocking this conversion of plasminogen to plasmin, the formed clot will be maintained.
You may be asking, why would there we be breaking down clots immediately after a traumatic event and bleeding. First, there is a constant balance of clotting and fibrinolysis in your body. Additionally, it seems intuitive, that is you suffer a wound that causes bleeding and your body corrects the bleeding, by forming a clot, it would not want to break it down till the area has healed. However, in severe trauma and injuries, there is a phenomenon called trauma induced coagulopathy (TIC) and acute traumatic coagulopathy (ATC). Both ATC and TIC are convoluted and still not completely understood.
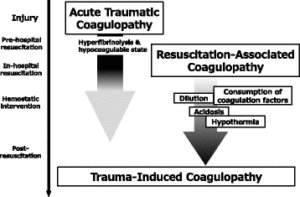
What is known, is there are many players in ATC and TIC. We know that fibrinogen is being consumed by the body much faster than usual. We also know, that if there is no resuscitation with blood or other drugs, prothrombin (precursor to thrombin) drops up to 20%, and thrombin is increased 1.5 times over first 4 hours. Finally, plasmin rises 2.5 times. Some scientist and physicians even believe that another protein involved in coagulation called activate protein C is the primary cause. This is unlikely, but as mentioned, it is a convoluted process that is not quite understood at this point.
If you are interested in a scientific discussion of ATC and TIC, here are two articles that review the concept:
https://www.ncbi.nlm.nih.gov/pubmed/28333829
In TCCC, TXA is used during the circulation (C) portion of the MARCH algorithm. The TXA indications per the TCCC guidelines are as follows:
“If a casualty is anticipated to need significant blood transfusion (for example: presents with hemorrhagic shock, one or more major amputations, penetrating torso trauma, or evidence of severe bleeding):
Administer 1 gm of tranexamic acid in 100 ml Normal Saline or Lactated Ringer’s as soon as possible but NOT later than 3 hours after injury. When given, TXA should be administered over 10 minutes by IV infusion. Begin the second infusion of 1 gm TXA after initial fluid resuscitation has been completed.”
The reason for the 10-minute infusion is due to issues of low blood pressure during a very large study called CRASH-2. Some argue that it can be pushed slowly in a 10-mL syringe over a few minutes. Because is prevents breakdown of clots and acts on blood, TXA should not be administered in the same line as blood or blood products.
Side effects include:
- Ocular – color vision change, vision loss
- Seizure – probably related to neuronal GABA inhibition
- Renal Impairment
- Ureteral Obstruction – upper tract obstruction may lead to bleeding
The contraindications for TXA:
- Acquired defective color vision
- Subarachnoid hemorrhage
- Active intravascular clotting
- Hypersensitivity to TXA
This sounds like a pretty awesome drug. Is it saving a lot of lives in combat? Let’s see that the studies say.
CRASH-2 this was a randomized and prospective study. It took place in 247 hospitals in 40 countries and had a lot of patients, that number is 20211 patients. The primary outcome measured was death at 4 weeks with intention to treat. The investigators found, that all causes of mortality decreased by 10%. Furthermore, the risk of death from bleeding decreased by 15%.
There were some who were not convinced that the CRASH-2 study was well done and had many flaws. Karim Brohi, a well-known trauma surgeon in the UK explains with humor why their assertions may be wrong here.
The military also investigated the use of TXA in combat. It was called the Military Application of Tranexamic Acid in Trauma Emergency Resuscitation (MATTERs) Study.
MATTERs was a retrospective, observational trial that compared TXA administration with non-TXA administration in combat casualties receiving at least 1unit blood. They also evaluated a subset of patients receiving a massive transfusion. They had 896 consecutive patients with combat wound, of which 293 received TXA. Their finding in the TXA group had lower mortality and it benefited patients receiving a massive transfusion. They said that TXA independently associated with survival.
That seems to be pretty good news for the combat wounded and even civilians…remember, this was in the civilian population first.
However, not everyone is convinced. There are physicians and scientists who are not so sure TXA is beneficial to everyone and in some cases, maybe harmful. Why does this happen? It may have to do with certain types of gene expression and/or the injury pattern. They are recommending to hold off on TXA until you can better identify who might benefit. This is determined in the emergency room. It is known, that giving TXA after three hours is harmful, there is no debate about that claim.
For now, TXA will remain a vital part of TCCC. It may have contributed to saving lives in combat since its implementation. Many EMS agencies around the country have implemented similar protocols to TCCC.
From a scientific standpoint, the best we can hope for is TXA is beneficial to most and at least not harmful to those where it is not beneficial. From a subjective and hopeful standpoint, it is cheap and easy to administer and hope it can help save more lives in combat. However, the jury is still out on TXA and its overall benefit in trauma patients.
_______________________
Andrew D. Fisher is now a medical student at Texas A&M College of Medicine after serving many years as a physician assistant with the U.S. Army. He joined the Army in 1993 as a Light Infantryman and spent three years at 1st Battalion, 75th Ranger Regiment before leaving the Army to pursue a college education. He is a 2006 graduate of the Interservice Physician Assistant Program. His previous assignments as a PA include UNCSB-JSA (Republic of Korea) and 1st Battalion, 75th Ranger Regiment. He has deployed seven times in support of the Global War on Terror/OCO. Andrew has taken care of more patients in the 75th Ranger Regiment than any other person since October 2001 and is the 2010 Army PA of the Year. Known as Old Man River, he is always angry, irritable, and cynical; at least it appears that way. He considers himself to be the least talented writer for the Havok Journal, but is very appreciative to have the opportunity. In his spare time he enjoys… who are we kidding, he has no spare time.
This article first appeared in The Havok Journal 23 August 2018.
© 2020 The Havok Journal
Like this article? Like us on Facebook!
havokjournal@havokmedia.com
The Havok Journal welcomes re-posting of our original content as long as it is done in compliance with our Terms of Use.
Buy Me A Coffee
The Havok Journal seeks to serve as a voice of the Veteran and First Responder communities through a focus on current affairs and articles of interest to the public in general, and the veteran community in particular. We strive to offer timely, current, and informative content, with the occasional piece focused on entertainment. We are continually expanding and striving to improve the readers’ experience.
© 2026 The Havok Journal
The Havok Journal welcomes re-posting of our original content as long as it is done in compliance with our Terms of Use.

