By Alex H.
Editor’s note: This essay is a first-person account from a Ukrainian servicemember. It is not medical advice. Readers experiencing unexplained pain, worsening wounds, infection symptoms, or post-blast injuries should seek professional medical care immediately. Some Ukrainian military terminology and medication names have been retained for authenticity and explained at the end.
***
There is a story making the rounds on social media about a person with no medical background who used ChatGPT to help develop a cancer vaccine for their dog.
I use AI myself. I use it for nutrition references, rehab exercises, and health monitoring. But I am writing this because my own experience should become a lesson for someone else.
If I had kept following AI when things became serious, I would probably be dead.
That is not drama. That is what my surgeon told me.
To explain what happened, I need to go back to early January, when I wrote about Russia-Ukraine War 2025: Russian Casualties and Historic Firsts.

The First Mistake
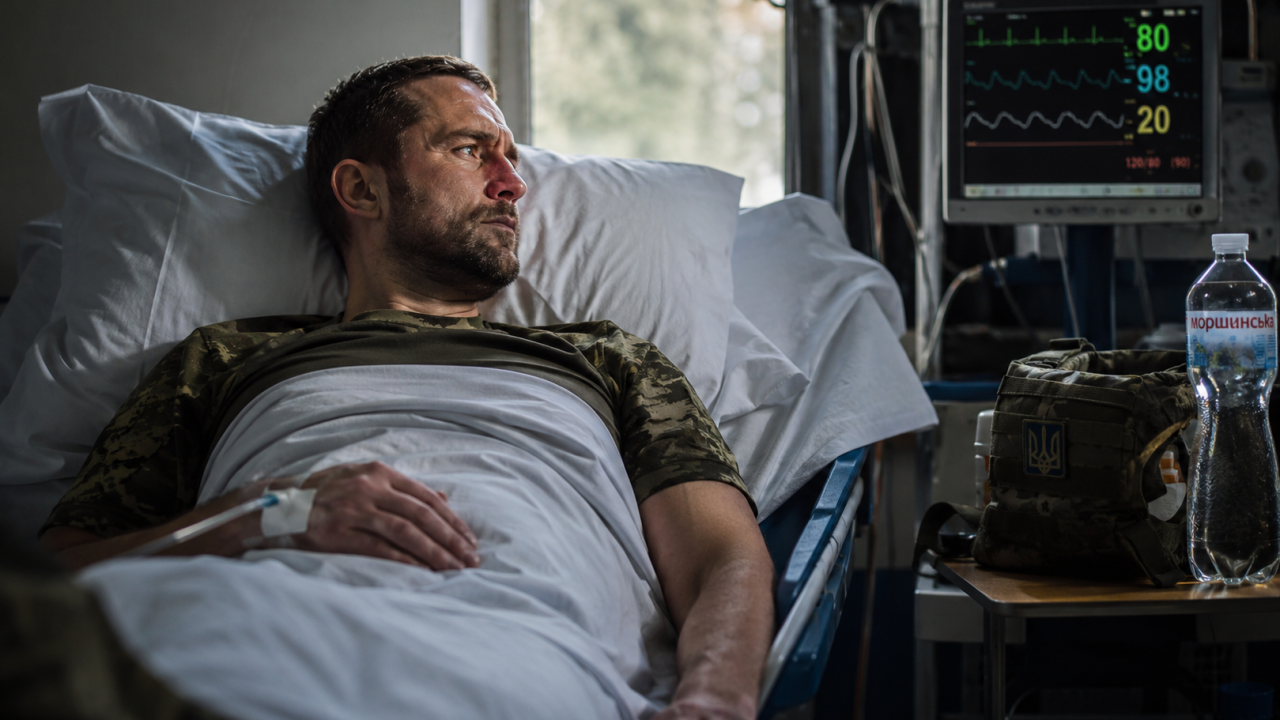
We were in Pokrovsk.
For several days, I had been freezing constantly. I had almost no desire to drink anything. No water. No tea. During breaks, I forced myself to eat a little porridge and some protein bars, but I was barely drinking at all.
That was the first mistake.
After another night in another basement, we were getting ready for a new day and new movement. Reconnaissance reported that the enemy might be watching the entrance to our building. That was confirmed when Russian troops were spotted in two buildings directly across from us.
We decided to jump out through the rear windows, circle around them, and give them a surprise.
As I jumped out in full kit, my right foot landed on a small rock. The foot rolled forward and my heel hit the frozen ground. My leg kept sliding on the ice. Reflexively, I put my left foot forward, loading it with my full body weight plus everything I was carrying.
I heard a distinctive crack, like tearing rubber.
Then the left leg gave out and I went down hard.
The movement happened without me, which was deeply frustrating. But after my combat medic examined me, it was clear I had a partial tear of the rectus femoris.
Fortunately, I had been carrying a small roll of kinesiology tape in my admin pouch for a long time. I keep it the way others keep a strip of reinforced duct tape. I taped my thigh so the tape would absorb some of the load, switched to stationary command mode, and stayed put.
Evacuation resources were stretched thin, and I was not going to burn them on myself when someone else might need them badly.
I went through everything I was carrying and stripped down as much weight as possible to take pressure off the leg and let it heal faster. That meant removing the ballistic shirt I had been wearing under my plate carrier.
That was the second mistake.

The Second Mistake
About a week later, at dusk, we were moving to another building.
I was still limping, but the leg felt noticeably better. I still was not carrying my normal load, and I still was not wearing the ballistic shirt.
Somewhere above us, we heard an FPV drone. Our RER operator warned us about Russian drones equipped with thermal optics.
The first two pairs sprinted to the target building, cleared it, and signaled that it was clear. After that, we crossed one at a time to reduce the risk of a drone taking out multiple people at once.
Halfway through my run, I heard the drone very close.
I jumped forward, trying to spin in the air and land on my back so I could control the space behind me. But you do not jump far on an injured leg.
The drone detonated behind me.
I felt the shock wave and a cloud of debris flying around me as I hit the ground. I checked the perimeter. Got up. Made it to the building.
Nobody was hurt that evening.
Almost nobody.
Once we set up positions, posted sentries and scouts, and started settling in for rest, I felt a weakness I was not used to. I started running my hands over my body and holding them up to the light, checking for blood.
On my lower right side, there it was. Not much. More like a scratch, with a small hole leaking slightly when I pressed on the surrounding tissue.
Pain level: two or three out of ten.
I told the medic. He came over. I took off the plate carrier and my clothes. It looked like a small graze with a tiny puncture. It leaked a little when pressure was applied around it.
We cleaned it. I applied pressure. We patched it.
Then we exhaled.

The Withdrawal
Another two and a half weeks passed.
We were working well, destroying seven to fifteen Russian troops per day with no losses of our own. Then the order came to withdraw.
This is always the hardest part of any deployment. Casualties on the way out are usually higher than at any other point. By the time you are leaving, you are already running on empty.
The first night of the withdrawal was the best one. A blizzard picked up and the temperature dropped further, so we used that window to move the most vulnerable people out first.
Then we waited.
More destruction of the enemy. Another window. Another movement.
Window by window, that was how it went.
The strongest were supposed to be last out. I left somewhere in the middle, and after that, every nerve and every bit of energy went into getting the others out safely.
Eventually, the last ones made it.
I collected all the paperwork and gear and drove to headquarters. Whether it was exhaustion or the tension finally unwinding, I had no appetite at all.
Somewhere on the road, I felt my battery dying. I stopped at a gas station and got a large Americano.
That evening, I felt discomfort around my pancreas and messaged the AI about it.

The AI Diagnosis
The AI response had all the hallmarks of confirmation bias.
It sounded like an observer trying to fit new information into an existing theory. It explained that the discomfort was caused by not eating and drinking black coffee on an empty stomach.
Its advice came down to three things: no food, plenty of water, and rest.
So I decided not to push through to headquarters that night. I stopped to rest.
I could not sleep.
By night, the discomfort had become pain. The AI suggested No-Spa and Almagel. My drone operator, who was traveling with us, had No-Spa in her kit, expired by a year. I took two tablets.
About an hour later, the pain eased slightly. That seemed to confirm what the AI and I had suspected about the pancreas.
But the discomfort did not go away.
The AI explained that this was simply because I did not have Almagel.
By morning, things were worse, and the next two tablets did nothing. The AI explained that the expired No-Spa was probably why it was not working.
Sunday morning. We stopped at the first pharmacy that opened after curfew. Fresh No-Spa and Almagel.
We drove on to Dnipro.
Things kept getting worse. Not unbearable. I could still hold myself together and hide how bad I felt. But there was no relief coming.
I asked the AI about taking a painkiller. It offered a cautious list.
I called a doctor I knew, described what I thought was pancreatitis, and asked about pain management options. He sent me straight to the hospital for a quick look, without waiting in line.
That was enough to convince me.
The problem was not that AI made one magical wrong diagnosis. The problem was worse than that.
It sounded reasonable. It matched what I already suspected. And every time the situation changed, it gave me another explanation that made delay feel rational.
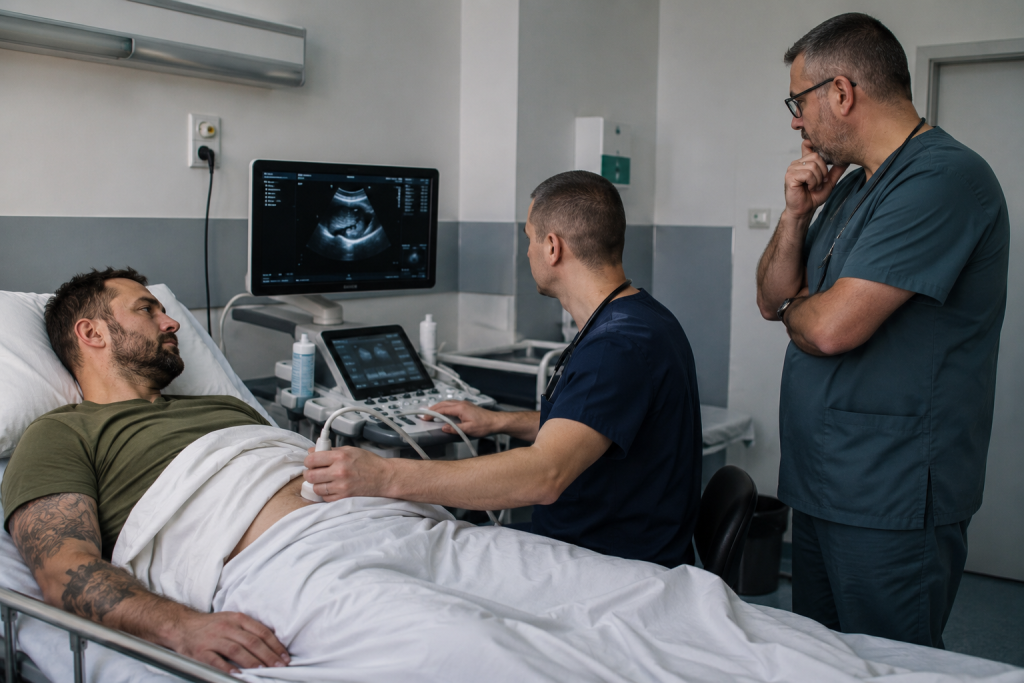
The Hospital
Physical examination. Referral for an ultrasound. Emergency ultrasound.
The radiologist reviewed the images and saw nothing immediately critical: a slightly enlarged pancreas, though not dramatically so; a slightly enlarged liver, but still within normal range; some gallstones; and abnormal inflammation on one side of the gallbladder.
Overall, nothing clearly pointed to a critical condition.
Referral to a surgeon. Emergency consultation with the surgeon.
He said the gallstones were most likely the source of my condition and proposed a laparoscopy to remove them.
I asked how long I would be out of action. He said possibly five to seven days, but first they needed to bring the pain down and run a course of IV drips to reduce the internal inflammation. That would take two days. Then we would make a decision.
Two days I could agree to.
They admitted me, processed the paperwork, ran a CT scan, chest X-ray, complete blood count, and ECG. They got me settled.
The whole time, I was getting worse.
Toward evening, they put in the first IV drip.
The AI was still explaining how this would help my pancreas.
At 5 a.m. the next day, another drip. My attending physician came by with no dietary restrictions from him. I ate whatever the nurse brought around for everyone.
That evening, another ultrasound and blood test. A different doctor confirmed the gallstone diagnosis.
Another drip.
The following morning, another drip. I was feeling noticeably better, though from the middle of the night I had trouble sleeping. Something felt like a bad mattress pressing into one spot in my back whenever I lay on it, so I kept shifting around.
My attending physician came for rounds. I told him I was feeling better overall. He said there was no critical threat to my health at that point and offered to let me decide for myself whether to go ahead with the laparoscopy.
By then, I had already briefed the commander on everything. I sent him photocopies of all reports, forms, and paperwork. I asked for until lunch to give the doctor an answer.
What I wanted was to get out of the hospital.
Naturally, I asked the AI.
Its response was something like this: since there was nothing critical, the surgery was not urgent.
I called the commander. He had taken over the complete withdrawal of my unit. Not part of it. All of it.
I still had some pain in my left thigh from the muscle tear, so I half-joked to myself: I might as well get rid of those stones while I am already useless, so I am not overloading the leg later.
If the operation meant five more days out of action at most, I would stay.
At lunch, I told the doctor.
He said surgery would be the following morning.
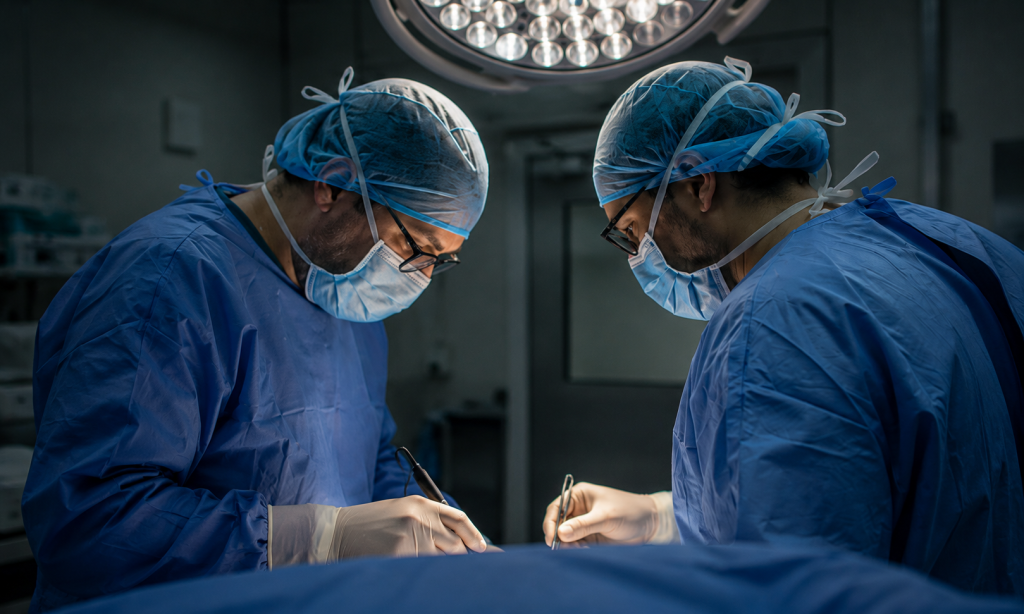
What the Surgeon Told Me
About five hours before the scheduled operation, things started getting worse.
Fast.
By the time they wheeled me into the operating room, I was at pain level ten.
Then anesthesia.
Relief.
Surgery.
The following morning, the surgeon who operated on me came by. I asked whether he had managed to get all the stones out.
He told me that the morning before the operation, I had developed peritonitis.
The gallbladder had ruptured. Bile and pus had spread across the entire peritoneal cavity.
If I had decided two days earlier to leave and drive back, within a few hours on the road I likely would have gone into septic shock: rapid blood pressure drop, kidney failure, loss of consciousness.
Not everyone in that condition makes it to a hospital in time.
“So what about the stones?” I asked.
He explained that they had been removed along with the gallbladder.
“Well,” I thought out loud, “that is one way to lighten the load on my leg.”
The surgeon believed the small fragment wound may have been the source of the internal infection. The wound we had treated as minor. The tiny hole from Pokrovsk. The one we cleaned, patched, and stopped thinking about.
It may have been the beginning of everything.
What I Took From It
Here is what I took from it:
- In cold weather, under load, and under stress, dehydration can sneak up on you. Do not treat hydration as optional.
- Additional soft-armor coverage matters. A ballistic shirt or similar protection can cover areas that a standard plate carrier leaves exposed. In my case, removing it was a mistake.
- There are no minor torso wounds in a combat zone. At the first opportunity, get a proper scan.
- My conclusion: combat deployments longer than two weeks without rotation become reckless, no matter how real the personnel shortages are.
- If I had followed the AI’s advice about my pancreas, managed the pain with medication, or decided against surgery, you might be reading an obituary right now.
- Painkillers are not treatment. They exist to buy time to get to a specialist. Nothing more.
- Do not diagnose yourself, even if you or someone close to you had something similar before. Similar symptoms can have completely different and far worse causes.
- Make decisions based on the worst-case scenario.
- You can make excuses your whole life. But life can end in minutes.
I hope this story pushes someone in my circle, a friend, or a reader to get checked if something has been bothering them and they have been putting it off.
Repeat after my surgeon:
“Not everyone in that condition makes it to a hospital in time.”
If you still have unfinished things, if there are people or animals who love you and whom you love, your excuse of “later” is not worth the risk.

Terms
Rehab: recovery exercises used to return a soldier or athlete to full training after injury.
RER: Ukrainian abbreviation for РадіоЕлектронна Розвідка, meaning signals intelligence, or SIGINT.
No-Spa: a brand name for drotaverine, an antispasmodic medication commonly used in Ukraine and other countries.
Almagel: an antacid medication.
CT: computed tomography.
ECG: electrocardiogram.
_____________________________
Alex H. is a Ukrainian servicemember writing under a pseudonym for operational security; his frontline analysis project is available at https://war-in-ukraine.com
As the Voice of the Veteran Community, The Havok Journal seeks to publish a variety of perspectives on a number of sensitive subjects. Unless specifically noted otherwise, nothing we publish is an official point of view of The Havok Journal or any part of the U.S. government.
Buy Me A Coffee
The Havok Journal seeks to serve as a voice of the Veteran and First Responder communities through a focus on current affairs and articles of interest to the public in general, and the veteran community in particular. We strive to offer timely, current, and informative content, with the occasional piece focused on entertainment. We are continually expanding and striving to improve the readers’ experience.
© 2026 The Havok Journal
The Havok Journal welcomes re-posting of our original content as long as it is done in compliance with our Terms of Use.